Racial discrimination in health care
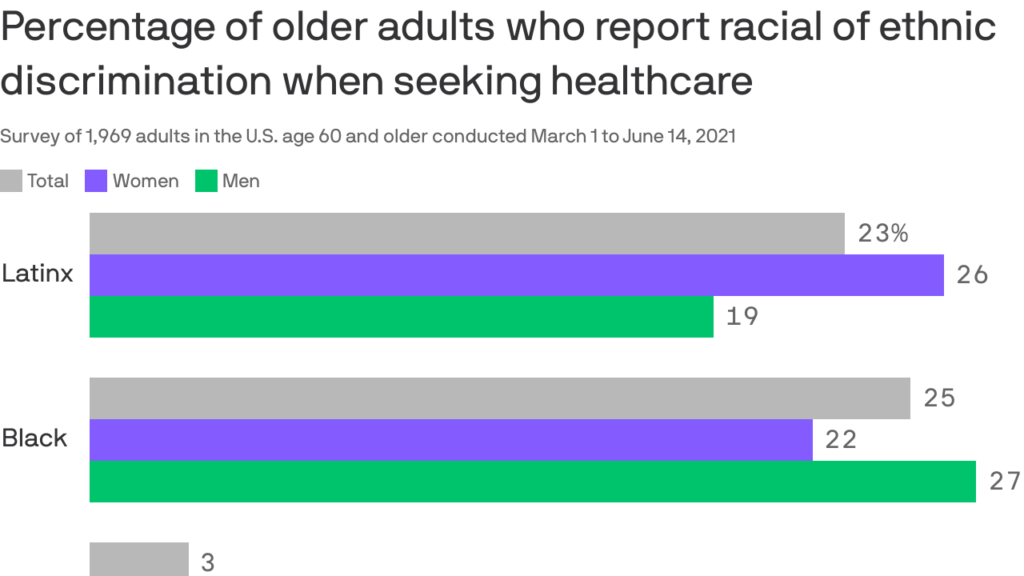
Racial discrimination in health care remains a persistent and systemic issue, deeply embedded in the structures of medical systems worldwide.
Despite advances in medicine and public health, marginalized racial and ethnic groups continue to experience disparities in access, treatment quality, and health outcomes. Studies consistently show that people of color are less likely to receive timely diagnoses, adequate pain management, and life-saving interventions compared to their white counterparts.
These inequities are fueled by implicit bias, socioeconomic factors, and historical injustices within the health care system. Addressing racial discrimination is not only a matter of ethics but a necessity for achieving true health equity.
 Is hugging sexual harassment
Is hugging sexual harassmentRacial Discrimination in Health Care: Systemic Inequities and Their Impact
Racial discrimination in health care is a persistent and deeply entrenched issue that affects millions of individuals across the United States and other multicultural societies. Despite advances in medical science and policies aimed at ensuring equitable treatment, people of color continue to experience significant disparities in access to care, quality of treatment, and health outcomes.
These inequities stem from a combination of implicit bias among health care providers, structural racism embedded in medical institutions, socioeconomic barriers, and historical mistrust due to past medical abuses, such as the Tuskegee Syphilis Study.
Marginalized communities, particularly Black, Indigenous, and Hispanic populations, often receive lower-quality care even when controlling for insurance status, income, and severity of conditions. This systemic discrimination contributes to higher rates of chronic illness, maternal mortality, and reduced life expectancy among racial minorities, highlighting the urgent need for comprehensive reform.
Implicit Bias and Provider Decision-Making
Implicit bias—unconscious attitudes or stereotypes that affect understanding, actions, or decisions—plays a critical role in racial discrimination within health care settings.
 Is sexual innuendo harassment
Is sexual innuendo harassmentNumerous studies have demonstrated that health care professionals often hold unconscious biases that lead them to perceive Black and other minority patients as less cooperative, exaggerating symptoms, or being less deserving of pain management.
For example, a landmark study published in the Proceedings of the National Academy of Sciences found that some medical trainees believed false biological myths, such as Black patients having thicker skin or less sensitive nerve endings, resulting in under-treatment of pain.
This type of bias can influence critical decisions regarding diagnosis, prescription of medication, and referrals for specialized care, ultimately contributing to worse health outcomes for patients of color, despite presenting with identical symptoms as their white counterparts.
Structural Barriers to Access and Treatment
Structural racism in health care manifests through systemic policies and institutional practices that limit access to high-quality medical services for racial minorities. Communities of color are more likely to reside in medically underserved areas with a scarcity of hospitals, clinics, and specialty care providers, a phenomenon known as health care deserts.
 What qualifies as sexual harassment
What qualifies as sexual harassmentMoreover, racial minorities are disproportionately uninsured or underinsured, limiting their ability to seek timely medical attention. Language barriers, lack of culturally competent care, and discriminatory practices in hospital admission or insurance coverage further exacerbate this inequity.
These structural factors result in delayed diagnoses, reduced screening rates for diseases like cancer, and lower rates of treatment adherence, ultimately widening the gap in health outcomes between racial groups.
Racial Disparities in Maternal and Infant Health
One of the most alarming examples of racial discrimination in health care is the stark disparity in maternal and infant mortality rates. Black women in the United States are three to four times more likely to die from pregnancy-related complications than white women, regardless of income or education level.
Even high-profile cases, such as those of Serena Williams and Simone Manuel, underscore how socioeconomic status does not shield Black women from being ignored or misdiagnosed during childbirth. This disparity reflects a combination of medical neglect, implicit bias, lack of access to prenatal care, and chronic stress due to systemic racism.
 Difference between harassment and sexual harassment
Difference between harassment and sexual harassmentSimilarly, Black and Indigenous infants face significantly higher mortality rates compared to white infants, pointing to systemic failures in perinatal care and early childhood health support for marginalized communities.
| Health Disparity | Racial Group Affected | Key Statistic | Contributing Factors |
|---|---|---|---|
| Maternal Mortality | Black Women | 3–4x higher than white women | Implicit bias, lack of prenatal care, medical dismissal |
| Chronic Disease Prevalence | Black and Hispanic Populations | Higher rates of diabetes, hypertension | Food deserts, lack of access to specialists, stress from racism |
| Pain Management Disparities | Black Patients | Less likely to receive opioid prescriptions | False beliefs about biological differences, implicit bias |
| Infant Mortality | Black and Indigenous Infants | 2x higher than white infants | Low birth weight, inadequate prenatal care, systemic neglect |
| Mental Health Access | Latino and Asian Communities | Lower treatment rates for depression/anxiety | Stigma, language barriers, lack of culturally competent providers |
Frequently Asked Questions
What is racial discrimination in health care?
Racial discrimination in health care refers to unequal treatment of patients based on their race or ethnicity. This can include differences in diagnosis, treatment options, pain management, and access to medical services.
Marginalized racial groups often receive lower quality care compared to white patients, even with similar health conditions and insurance. These disparities result from both systemic biases and individual prejudices within the health care system.
How does racial discrimination affect health outcomes?
Racial discrimination in health care leads to worse health outcomes for minority populations. Studies show that Black, Indigenous, and other people of color experience higher rates of chronic illness, maternal mortality, and preventable deaths.
 Difference between sexual assault and harassment
Difference between sexual assault and harassmentDelayed diagnoses, inadequate treatment, and lack of trust in providers contribute to these disparities. Ongoing stress from discrimination also negatively impacts mental and physical health, worsening overall well-being and life expectancy in affected communities.
What are examples of racial bias in medical treatment?
Examples include underestimating pain in Black patients, assuming they have higher pain tolerance, and less frequently prescribing pain medication. Women of color, especially Black and Native American women, face higher risks during childbirth due to ignored symptoms and delayed interventions.
Minority patients are also less likely to be referred for specialist care or advanced treatments. These biases often stem from outdated medical beliefs and lack of cultural competence among providers.
What can be done to reduce racial discrimination in health care?
To reduce discrimination, health care systems must implement anti-bias training, improve diversity among medical staff, and enforce equitable policies. Collecting and analyzing race-based health data helps identify disparities.
Ensuring language access and culturally competent care improves patient trust. Hospitals should adopt standardized treatment protocols to minimize subjective decision-making. Systemic changes, including policy reform and community engagement, are essential for creating fair and inclusive health care for all.

Leave a Reply